Safe Medications to Use During Gestational Diabetes
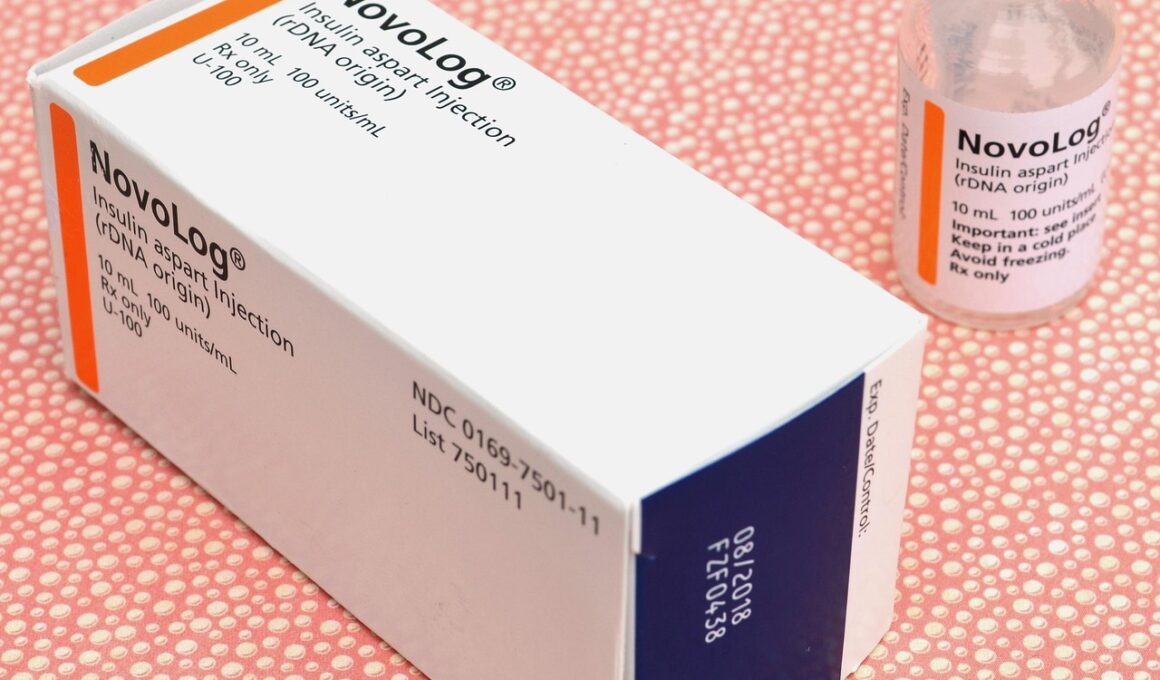
Managing gestational diabetes is crucial for the health of both mother and child. This condition can often be regulated through dietary changes and exercise. However, in some cases, medications may be necessary. It’s essential to consult with healthcare professionals to determine the best course of action. In general, insulin is the primary medication prescribed, as it is safe for both the mother and fetus. It helps to lower blood glucose levels effectively. Oral medications like metformin may also be utilized, but must be evaluated carefully. Pregnant women should never self-prescribe and must seek proper medical advice. Monitoring blood sugar levels regularly is also important. This helps determine if medication is required, or if lifestyle changes are sufficient. Pregnant women should educate themselves about their options. Understanding safe medications and their implications is key. With guidance, women can manage gestational diabetes effectively and minimize risks. Finally, always discuss any concerns with a healthcare provider to ensure the best outcomes for both mother and baby.
Insulin therapy is often the first-line treatment option for gestational diabetes. It plays an essential role in normalizing blood sugar levels throughout pregnancy. Insulin is not harmful to the developing fetus, making it a widely accepted choice. It is administered through injections, and dosage is adjusted based on the patient’s blood sugar readings. Patients should receive education on how to administer insulin and monitor glucose levels effectively. In addition, pregnant women should maintain a healthy diet that complements their insulin management. Regular check-ups with healthcare professionals are crucial to track progress. Alternatives to insulin therapy include oral medications, such as metformin and glyburide. Metformin helps in reducing insulin resistance, promoting better glucose control. Glyburide, on the other hand, stimulates insulin release from the pancreas. These medications may be suitable for some mothers, but safety must be assessed individually. Furthermore, ongoing research is crucial to evaluating the effects of these medications. Continuous consultation with healthcare providers can help ensure that treatment approaches remain appropriate. Using medication safely during pregnancy is paramount.
Importance of Monitoring Blood Sugar
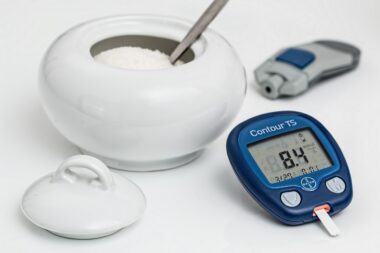
Monitoring blood sugar levels is paramount for managing gestational diabetes. Regular checks help to keep track of how food, activity, and medication affect blood glucose. This vital practice enables expectant mothers to maintain their glucose levels within normal ranges. Elevated blood sugar can lead to complications for both mother and child. Women should familiarize themselves with the monitoring process, including using a glucometer. Finding the right times to check blood sugar levels can make a significant difference in management. Generally, blood sugar should be monitored before meals and after eating to better understand patterns. It’s also advised to keep a log of daily readings to discuss with healthcare teams. This data provides essential insights that allow for personalized management plans. Emphasis on maintaining target levels is critical to pregnancy outcomes. If blood sugar levels rise too high, adjustments may be required in medication or lifestyle. Women may also receive support from certified diabetes educators and nutritionists. Overall, monitoring is a crucial strategy in the effective management of gestational diabetes.
Diet plays an essential role in managing gestational diabetes effectively. A well-balanced, nutritious diet helps stabilize blood sugar levels. Pregnant women should focus on consuming whole foods, including vegetables, fruits, lean proteins, and whole grains. These foods provide essential nutrients while maintaining adequate blood sugar levels. It’s important to understand carbohydrate counting and complex versus simple carbs. Complex carbohydrates release glucose more slowly, providing more stable energy levels. Monitoring portion sizes is equally important to avoid spikes in blood sugar. Additionally, regular meal timing helps prevent extreme fluctuations. Make sure to incorporate activities such as light exercise into daily routines. Exercise can improve insulin sensitivity, helping to manage blood glucose levels better. Consultation with dietitians specializing in gestational diabetes can also guide meal planning. They can create individualized meal plans suited to specific preferences and requirements. Staying hydrated is another significant part of dietary management. Drinking plenty of water helps in overall metabolic functions. Together, these dietary practices help support a healthy pregnancy while managing gestational diabetes effectively.
Potential Complications of Unmanaged Gestational Diabetes
Unmanaged gestational diabetes poses significant risks for mothers and their unborn babies. Elevated blood glucose levels can lead to serious complications during pregnancy and delivery. For the mother, risks include preeclampsia, a serious condition characterized by high blood pressure. Additionally, there is an increased likelihood of cesarean delivery due to larger fetal size, known as macrosomia. For the baby, potential complications include higher birth weights, resulting in delivery challenges. Babies born to mothers with unmanaged diabetes may also face neonatal hypoglycemia or low blood sugar levels after birth. Furthermore, these infants may develop an increased risk of obesity and type 2 diabetes later in life. Continuous monitoring and appropriate medication can help mitigate these risks effectively. Choosing a healthy lifestyle with proper nutritional guidance is equally essential to maintain blood sugar levels. Regular consultations with healthcare providers are critical to ensure that both mother and baby remain healthy. With informed management, many women can successfully navigate gestational diabetes without complications. Thus, proactive approaches can lead to positive outcomes for mothers and babies. Good prenatal care ultimately contributes to a healthier future for the entire family.
Emotional well-being is another crucial aspect of managing gestational diabetes. Pregnancy can be a time of heightened emotions, especially when health concerns arise. The diagnosis of gestational diabetes can sometimes lead to anxiety and stress. Women must prioritize mental health alongside physical health. Support systems play an important role in addressing emotional challenges. Family, friends, and healthcare providers can offer encouragement and guidance. Participating in support groups specifically designed for expectant mothers can also provide valuable emotional relief. Sharing experiences with others facing similar challenges can significantly empower women. Additionally, practicing stress-reduction techniques, such as mindfulness and relaxation exercises, can greatly enhance emotional well-being. Taking time for self-care and engaging in enjoyable activities can help alleviate stress. It’s crucial for women to express their feelings and seek help when needed. Open communication with healthcare providers regarding emotional struggles can lead to additional support, such as counseling or therapy. Addressing mental health is just as important as managing diet and medication. By acknowledging emotional aspects, mothers can create a more balanced approach towards their health during pregnancy.
Conclusion: Managing Gestational Diabetes
In conclusion, managing gestational diabetes effectively requires a multifaceted approach. Through proper medication, dietary choices, and emotional support, women can maintain healthier pregnancies. Navigating this condition is achievable with the right resources and guidance from healthcare professionals. Women should actively monitor their blood sugar levels and adhere to treatment plans prescribed by their healthcare providers. Moreover, a supportive network of family, friends, and healthcare members can lend invaluable assistance. Incorporating healthy lifestyle changes contributes to their overall well-being and helps control blood glucose levels. It’s vital to remain informed about potential complications and recognize signs that require immediate medical attention. Continuous education empowers mothers and supports their health goals during pregnancy. Furthermore, post-delivery care is essential for all women diagnosed with gestational diabetes. Regular follow-ups enable healthcare teams to assess long-term risks and help in preventing the onset of type 2 diabetes later in life. Ultimately, managing gestational diabetes successfully leads to healthier outcomes for both mother and child. Investing time and effort into this management will yield significant dividends in the family’s overall health and happiness.
Maintaining good health throughout pregnancy is of utmost importance. The journey through gestational diabetes can be daunting, but with proactive management strategies in place, it can lead to positive outcomes. Emphasis on safe medications, proper diet, emotional support, and regular monitoring are key components of this journey. With diligent care and guidance, mothers can navigate this period effectively, ensuring the best possible environment for their developing baby, ultimately leading to a healthier future for both.