Glossary of Blood Sugar Monitoring Terms
Understanding the various terminologies related to blood sugar monitoring is crucial for managing diabetes effectively. Here are some essential terms you should know. Blood Glucose Level: This refers to the amount of glucose present in the blood at any given time. It’s vital to monitor these levels to ensure they stay within a healthy range. Hypoglycemia: This condition occurs when blood glucose levels drop dangerously low, often leading to symptoms like dizziness, sweating, or confusion. Individuals should learn the signs to act quickly. Hyperglycemia: Opposite of hypoglycemia, this term describes high blood glucose levels that can be harmful and require intervention. Continuous Glucose Monitor (CGM): A device that checks glucose levels continuously throughout the day. It provides crucial insights into how food, activity, and medications affect glucose levels consistently. Fasting Blood Sugar: This measurement is taken after an overnight fast, determining the baseline level of glucose, which is vital for diagnosing diabetes.
The term HbA1c: is another critical concept in the diabetes management glossary. It measures the average blood glucose levels over the past two to three months, providing insights into long-term blood sugar management. Generally, an HbA1c level below 6.5% is considered normal and indicates good control. A higher percentage might suggest poor management of diabetes, making it crucial for health assessments. Self-Monitoring of Blood Glucose (SMBG): This refers to the practice where individuals with diabetes regularly check their blood glucose levels at home using a glucose meter. Regular monitoring can yield important data to help make informed decisions regarding treatment and lifestyle. Insulin Sensitivity: This is how responsive your body is to insulin, influencing blood sugar control. An increase in insulin sensitivity can lower blood glucose levels. Carbohydrate Counting: A method used to track carbohydrate intake to help manage blood sugar levels effectively. Individuals learning carbohydrate counting can plan their meals better to ensure balanced glucose levels.
Insulin and Its Types
Insulin is a hormone critical for managing diabetes. Rapid-Acting Insulin: This type starts working within minutes and is typically used around mealtimes to manage blood sugar spikes. Knowing effective timing for administration is essential for optimal results. Long-Acting Insulin: This variety releases insulin slowly over time, helping to maintain steady blood glucose levels throughout the day or night. Basal Insulin: Refers to the consistent level of insulin your body needs when not eating. Maintaining baseline insulin levels is crucial for stable glucose control. Prandial Insulin: This is taken during mealtimes to help manage the increase in blood sugars caused by food intake. Learning about insulin types is vital for proper management. Understanding how and when to use these different types of insulin is necessary for effective diabetes control, ensuring individuals can adjust their dosages based on lifestyle factors, meals, and activity levels.
Another important term to consider is Glucose Tolerance Test (GTT): This test assesses how well the body processes glucose and is essential for diagnosing conditions like prediabetes and diabetes. Individuals drink a glucose solution, and blood samples are taken over time to measure glucose levels. Continuous Glucose Monitoring System: A CGM system offers real-time glucose measurements, allowing users to observe trends and patterns, making it easier to manage diabetes effectively. Diabetic Ketoacidosis (DKA): A severe complication arising from high blood sugar levels that can occur when the body doesn’t have enough insulin, leading to the production of ketones, which can be dangerous. Glucose Variability: This term defines the fluctuations in blood glucose levels throughout the day, which can impact overall diabetes management. Understanding these metrics helps in narrowing down what is normal for each individual, enhancing personalized care.
Monitoring Devices
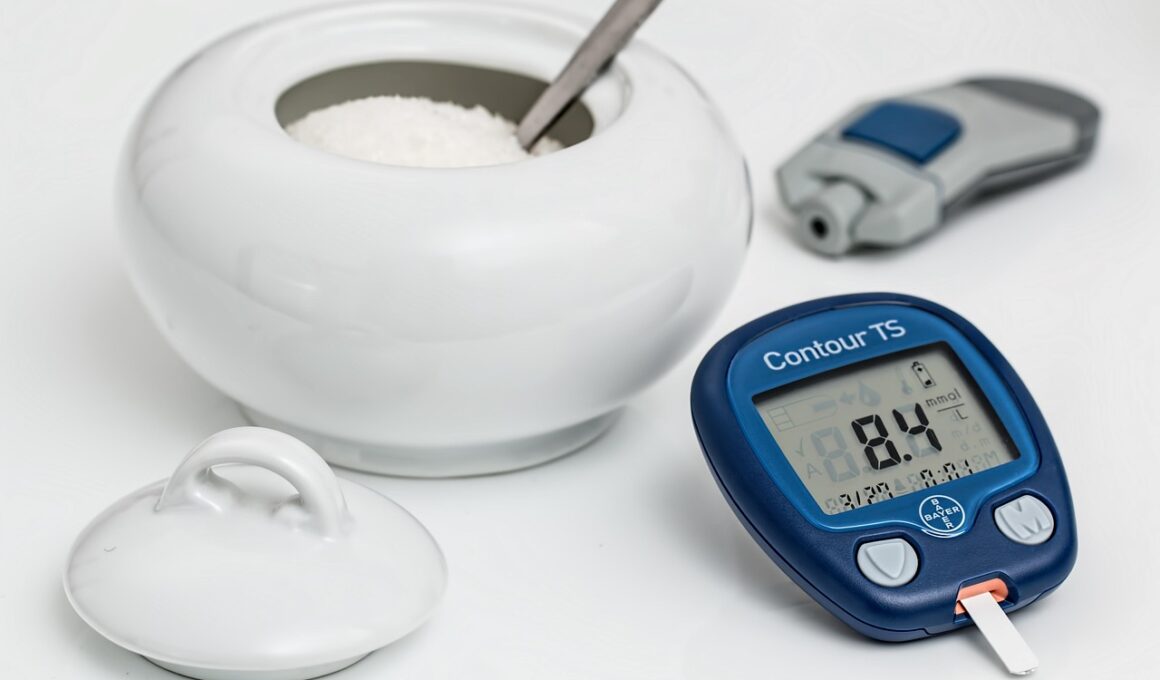
Many monitoring devices help manage diabetes effectively. Blood Glucose Meter: A fundamental device that measures blood glucose levels through a small blood sample, providing immediate results that help track daily patterns. Learning proper use is crucial for accuracy. Another essential device is the Flash Glucose Monitoring system: This innovative technology allows users to scan a sensor placed on the skin to get a glucose reading. It provides an alternative to traditional finger-pricking methods. Insulin Pen: This convenient device delivers precise insulin dosages comfortably and easily. Knowing how to use an insulin pen correctly is vital for diabetes management. Wearable Technology: Newly emerging technologies include smartwatches and other gadgets that track physical activity and heart rate, assisting in managing diabetes by providing insights into how exercise impacts blood sugar levels.
Another beneficial term is Low Glycemic Index (GI): Foods with a low glycemic index raise blood sugar levels slowly, making them beneficial for individuals with diabetes. Examples include most fruits, vegetables, and whole grains. Dietary Fiber: This is a vital component in blood sugar management as it aids in digestion and helps maintain stable glucose levels by slowing glucose absorption. Individuals are encouraged to incorporate high-fiber foods like legumes, nuts, and seeds into their diets. Meal Planning: This practice involves organizing meals ahead of time to ensure balanced, nutritious intake that aligns with personalized glucose goals. Planning meals allows greater control over blood sugar levels. Glycemic Load: This measures the total glycemic impact of a food item based on the amount consumed, providing further insights into how certain foods can affect blood sugar levels.
Healthcare Guidance
Finally, consistent interaction with healthcare professionals is essential. Endocrinologist: This specialized physician focuses on hormone-related issues, including diabetes management. Regular appointments with an endocrinologist can help tailor a more effective management plan. Dietitian: A registered dietitian can provide invaluable dietary advice tailored to individual diabetes needs, helping to create meal plans to stabilize blood sugar. CDE (Certified Diabetes Educator): This health professional can educate and support individuals in managing their diabetes effectively. This guidance helps patients with daily management strategies and adjustments. Support Groups: Being part of a community can provide emotional support and shared experiences around diabetes management.
Each term in the glossary serves a purpose in the overall understanding and management of diabetes. By becoming familiar with blood sugar monitoring terms, individuals can enhance their self-management skills and improve their quality of life. Knowledge is critical, enabling individuals to communicate effectively with healthcare providers. Empowerment through education can lead to better control and fewer complications, leading to a healthier lifestyle overall. Adopting a proactive approach towards diabetes management is essential for living a full, active life. Collaboration with healthcare professionals, paired with a solid understanding of monitoring terminology, paves the way for effective management. Staying informed about technology and advancements in diabetes care ensures that individuals are equipped with the resources necessary for success. Further research into new devices, medications, and management strategies continues to evolve, contributing to the overall well-being of those living with diabetes. In conclusion, the glossary of blood sugar monitoring terms is a vital resource for anyone affected by diabetes. Individuals can effectively navigate their journey with diabetes through continued learning and adaptation.