The History and Evolution of Dry Needling Practices
Dry needling has its origins rooted in traditional Chinese medicine, where various forms were utilized for pain relief and muscle tension management. However, the modern practice began gaining traction in the 20th century, spearheaded by physical therapists. They recognized the therapeutic benefits of inserting thin needles into trigger points to alleviate pain and improve muscle function. Initially viewed with skepticism by both medical practitioners and patients, dry needling has evolved significantly over the decades. It combines Western anatomical knowledge with traditional acupuncture principles. As practitioners gained greater understanding of myofascial pain syndromes, dry needling emerged as an innovative technique for addressing neuromuscular conditions. The development of educational programs and training courses has facilitated wider acceptance and understanding among healthcare providers. Moreover, research studies began to support its effectiveness, further legitimizing the practice within physical therapy. Over time, dry needling has become a legal treatment modality in many countries, expanding its reach across diverse healthcare settings. This evolution illustrates how dry needling bridged the gap between ancient practices and modern therapeutic techniques, fostering a deeper appreciation for holistic patient care in physical therapy.
As dry needling practices emerged, several studies highlighted its efficacy for various conditions, paving the way for a more widespread adoption. Several clinical trials demonstrated its positive impact on conditions such as chronic pain, muscle stiffness, and sports injuries. Different techniques, such as superficial or deep needling, were developed to address varied patient needs. The differentiation allowed practitioners to customize treatments to specific ailments more effectively. Consequently, specific protocols and guidelines began shaping how therapists approached this technique. The establishment of regulatory organizations provided practitioners with a framework to ensure safe and effective application of dry needling. Continuous research into the physiological effects of needle insertions yielded valuable insights, enabling physical therapists to implement evidence-based practices. Patient feedback played a crucial role too, as individuals reported improvements in their pain levels and overall well-being. As more evidence surfaced, healthcare professionals increasingly began collaborating to integrate dry needling into multidisciplinary treatment plans. Learning from various disciplines enriched physical therapy practices, promoting further exploration of this technique’s potential uses in chronic pain management, rehabilitation, and athletic performance enhancement.
The Science Behind Dry Needling
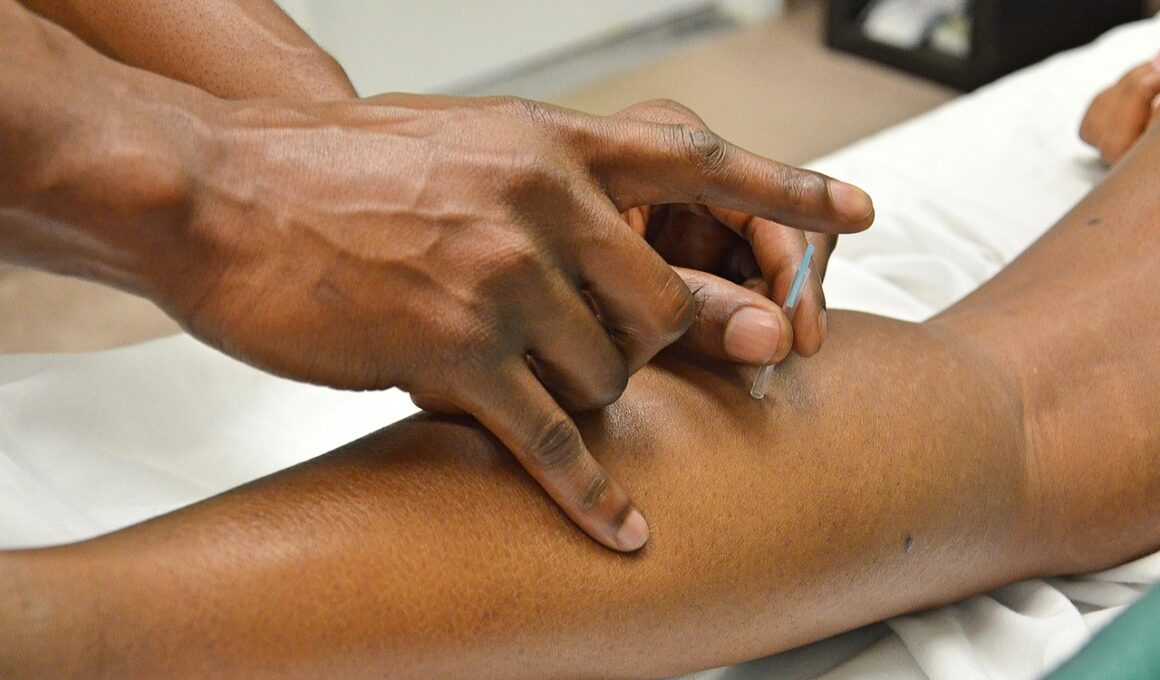
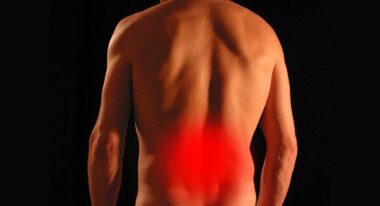
In understanding dry needling, it’s essential to explore its scientific foundations. By inserting needles into trigger points, physical therapists aim to reduce muscle tension, alleviate pain, and restore function. Trigger points are localized areas of muscle that are hyper-irritable and can refer pain to other areas. This phenomenon is known as referred pain, leading to misunderstandings regarding the source of discomfort. Dry needling aims to deactivate these trigger points, improving circulation, decreasing inflammation, and promoting healing. The needle induces a ‘twitch response,’ leading to a release of pent-up tension in the muscle. Studies have shown that this mechanistic approach can activate the body’s natural pain relief mechanisms, such as the release of endorphins and altering pain perception. Furthermore, dry needling may also influence local neurophysiological pathways, disrupting pain signals sent to the brain. Research continues to examine the physiological effects and optimal techniques to maximize benefits. Practitioners rely on a detailed assessment to determine appropriate treatment parameters, including target areas and needle depths, ensuring the most effective outcomes for their patients.
While dry needling showcases significant benefits, it also presents challenges and controversies that practitioners face. Some argue that it lacks sufficient scientific backing, particularly in the context of varied treatment protocols. Additionally, there is a discrepancy between the training and skill levels of practitioners offering dry needling techniques. In some regions, therapists may not require extensive education before administering this treatment, raising concerns regarding patient safety. Consequently, the establishment of stringent training programs has become essential to ensure proper application and avoid possible complications. Addressing these controversies necessitates further rigorous research that could strengthen the evidence base surrounding dry needling practices. Organizations and practitioners must advocate for high standards and increased education across the board. Another challenge is the misconception surrounding dry needling and acupuncture. Despite their similarities, they are distinct practices with differing theoretical foundations. Educating patients about these differences is vital for informed consent and realistic expectations. Ultimately, strengthening the credibility of dry needling and ensuring patient safety will foster a more comprehensive understanding of the treatment amongst both practitioners and the public.
Integrating Dry Needling into Contemporary Physical Therapy
Dry needling is now recognized as an essential component within contemporary physical therapy settings, augmenting traditional methodologies. Many therapists incorporate dry needling alongside other treatment modalities, such as manual therapy and therapeutic exercises, creating well-rounded care plans for their patients. The interplay between these various techniques facilitates better outcomes for individuals suffering from musculoskeletal pain and dysfunction. As practitioners embrace this integrative approach, the popularity of dry needling continues to rise, particularly among sports medicine professionals and rehabilitation specialists. Due to its effectiveness in treating sports-related injuries, athletes have increasingly turned to dry needling as part of their recovery protocol. Additionally, the demand for this technique has led to the establishment of specialized clinics dedicated to advanced pain management. The adaptability of dry needling extends its applicability from chronic pain management to acute sports injuries and post-operative rehabilitation. As physical therapists refine their skills through ongoing education, the integration of dry needling into practice enhances patient outcomes and promotes a holistic approach to wellness. Patients are likely to experience a heightened sense of autonomy and empowerment throughout their recovery journey.
Today, the future of dry needling appears promising as more professionals adopt the technique. The growing acceptance of dry needling is mirrored across various settings, from outpatient services to hospital systems. This trend reflects an increasing awareness of alternative methods in managing pain without relying solely on pharmacological interventions. The involvement of educational institutions in developing comprehensive training programs ensures that physical therapists are equipped with the necessary skills. Research continues to explore the long-term effects of dry needling, focusing on the quality of life improvements among patients. Innovative methods may arise, further expanding the therapeutic scope of dry needling, including new techniques for specific populations. In addition to classical approaches, the exploration of combining dry needling with complementary therapies shows great potential. Collaborations between professionals across disciplines will enhance understanding and further validate the effectiveness of dry needling. Advocacy for patient education regarding treatment choices will empower individuals to make informed decisions. As this practice evolves, dry needling may effectively revolutionize physical therapy and redefine how clinicians approach pain management in the future.
Conclusion: The Journey of Dry Needling
In conclusion, the history of dry needling reflects the journey of a practice transforming from traditional methods to a recognized therapeutic modality. Its evolution illustrates the fusion of ancient wisdom and modern techniques within physical therapy. The extensive research supporting dry needling’s efficacy emphasizes the importance placed on evidence-based practice in healthcare. As education and guidance surrounding dry needling progresses, patients stand to benefit greatly. Greater outreach regardless of demographic or geographic barriers will help raise awareness, leading to broader access to dry needling therapies. The successful integration of dry needling techniques into physical therapy practice encourages collaboration among healthcare providers, fostering a holistic treatment approach. Looking ahead, practitioners must continue to explore innovative techniques while addressing challenges. The collaboration between researchers, educators, and practitioners is vital to uphold the integrity and efficacy of dry needling practices. Ultimately, the transformative journey of dry needling within physical therapy serves as a testament to the potential for holistic healing through informed, innovative, and integrated patient-centered care practices.
As dry needling becomes mainstream, patient education will be paramount in ensuring a positive therapeutic experience. Providing clear information regarding the process, expected outcomes, and possible side effects will equip patients with realistic expectations. Moreover, as individuals share their experiences and successes, an increased awareness will drive demand for skilled practitioners. Harnessing patient testimonials and scientific evidence can further legitimize the practice within the healthcare community. Social media platforms provide a unique opportunity to create discussions around dry needling, promoting benefits while addressing common concerns. As professionals contribute meaningful content, cultivating a strong online presence will foster trust and credibility amongst potential patients. Additionally, enhancing interdisciplinary collaboration will strengthen the knowledge base and encourage the integration of dry needling into comprehensive treatment plans. In doing so, healthcare providers can harness each other’s strengths to create optimal strategies for managing complex pain conditions. As this field enters an exciting new chapter, the relationship between dry needling and physical therapy highlights the dynamism of contemporary healing practices. The evolution of dry needling symbolizes adaptability, emphasizing the importance of continuous education and open dialogue in shaping the future of patient care.