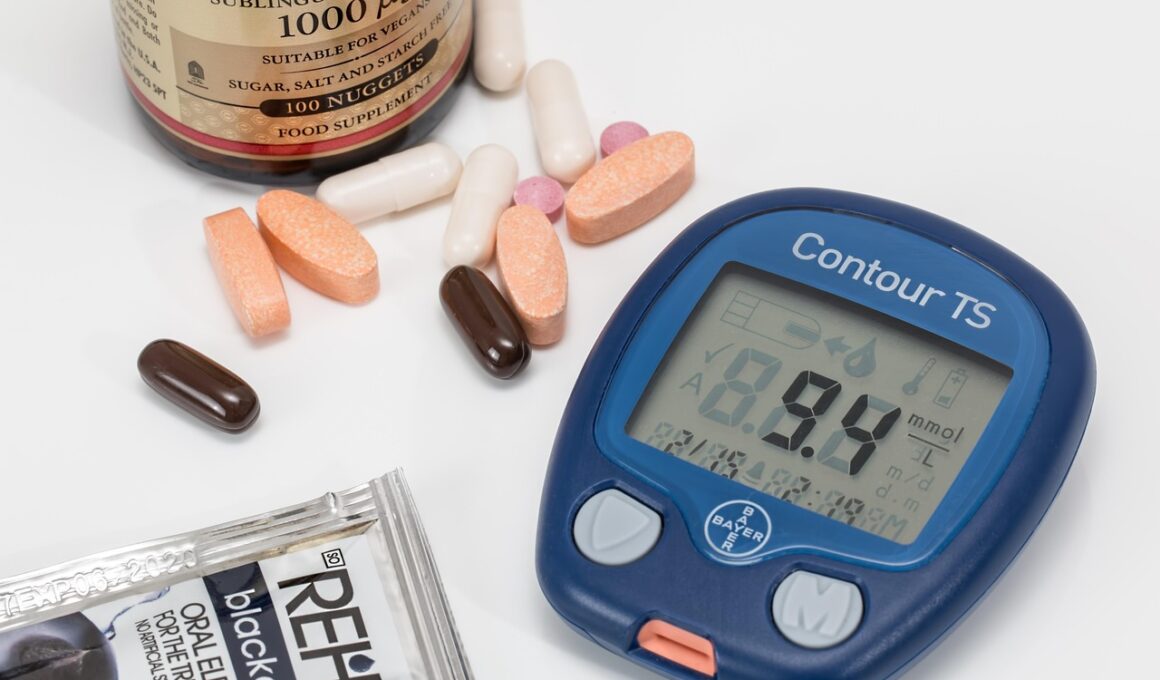
Vitamin Supplements and Diabetic Retinopathy: Fact vs. Fiction
Diabetic retinopathy is a significant complication that affects individuals with diabetes, potentially leading to blindness. Many people search for solutions or treatments, including the use of vitamin supplements. However, there is much confusion surrounding the effectiveness of these vitamins for preventing or treating retinopathy. The available scientific literature indicates that while certain vitamins may support overall eye health, they are not a substitute for conventional medical treatments. For instance, antioxidants such as vitamin C and E have been studied for their protective roles against oxidative stress, though definitive conclusions about their impact on diabetic retinopathy are still pending. Proper management of diabetes, including blood sugar control, remains critical in reducing the risk of this eye disease. Alongside medications, a balanced diet rich in whole foods, fruits, and vegetables can also contribute positively to eye health. Consult with healthcare providers regarding supplements before starting any regimen, as excessive intake may lead to adverse effects. It is important to engage in regular eye exams to monitor eye health effectively, allowing for early intervention if diabetic retinopathy develops. Learn more here.
The Role of Vitamins in Eye Health
A common misconception is that vitamin supplements can fully protect against diabetic retinopathy. Vitamins play a significant role in maintaining overall eye health; however, they should not be seen as a stand-alone treatment. For instance, vitamins A, C, and E are vital for vision and may help protect against age-related eye diseases. However, when it comes to diabetic retinopathy specifically, research findings suggest their effects may not be sufficiently robust on their own. Oxidative stress is often a contributing factor to diabetic complications, making antioxidants particularly interesting. Some studies show potential benefits of certain antioxidant vitamins in reducing the risk or progression of diabetic retinopathy. Nonetheless, conflicting results across various research efforts highlight that while they may confer some benefits, they shouldn’t be considered a primary treatment option. Furthermore, the importance of lifestyle factors, such as regular exercise and maintaining healthy blood sugar levels, cannot be overstated. Thus, incorporating a comprehensive approach—diet, vitamin intake, and medical treatment—proves more beneficial for managing this eye complication adequately.
Engaging in regular physical activity, along with adhering to dietary recommendations, can profoundly affect diabetes management and eye health. In recent years, studies have demonstrated that exercise contributes positively to glucose metabolism and overall well-being. Importantly for patients with diabetes, regular physical activity can help stabilize blood sugar levels, thereby reducing the risk of complications such as diabetic retinopathy. Beyond blood sugar control, exercise may also enhance circulation and support eye health through improved blood flow to the retina. Combining a healthy workout regime with a balanced diet rich in essential nutrients creates a synergistic effect that can benefit those at risk of diabetic complications. While vitamin supplements might assist in providing necessary nutrients, they should complement, rather than replace, a healthy lifestyle. Patients should consult with healthcare professionals before starting any new supplementation, especially individuals managing diabetes with existing retinopathy. Ultimately, a multidisciplinary approach, engaging dieticians, exercise specialists, and ophthalmologists, will offer more comprehensive outcomes for diabetes patients. Prevention strategies remain a collective responsibility for patients, caregivers, and healthcare providers.
Scientific Evidence and Ongoing Research
Recent scientific inquiries into the role of vitamins in the context of diabetic retinopathy have yielded mixed results. Some trials have highlighted potential benefits, while others have shown negligible effects from vitamin supplementation. For instance, the AREDS (Age-Related Eye Disease Study) suggests that a specific formulation of vitamins can reduce the progression of macular degeneration, but such outcomes are different from those for diabetic retinopathy. Thus, the translation of these findings to diabetic patients can be complex. Additionally, it is essential to emphasize that while vitamins might play a role, they are not replacements for prescribed drug therapies like anti-VEGF injections. A growing body of research focuses on the interplay of diabetes, nutritional intake, and ocular health to clarify these relationships. Ultimately, ongoing studies aim to devise practical recommendations tailored for individuals with diabetes. They explore not just vitamins, but also other potential nutritional supplements and their combined effects. Engaging patients and clinicians in understanding these dynamics will offer a broader comprehension of managing diabetic complications through diet and lifestyle.
Often, the communication regarding dietary supplements in clinical settings can be vague. Patients may receive mixed messages about the importance of vitamins without sufficient emphasis on their actual efficacy concerning diabetic retinopathy. This problem underscores the necessity for clearer guidelines from health professionals on this topic. Patients keenly interested in vitamin supplements can sometimes overlook essential components of eye care, such as regular eye examinations and fundamental diabetes management practices. Medical professionals should strive to educate patients on the crucial factors contributing to eye health. Moreover, discussions on supplements should also address potential side effects and the importance of achieving a balanced nutrient intake through food. The role of education in diabetes self-management cannot be overstated, as informed patients tend to make better health choices. Accessible resources, workshops, and consultations can help demystify the subject of vitamins and supplements. By fostering informed discussions, patients can better understand their condition and the role nutrition plays in their therapy. Consulting specialists, including registered dieticians and diabetic educators, can further empower patients in their journey toward better health.
Conclusive Insights
While vitamin supplements can contribute to general health and well-being, their role in preventing or treating diabetic retinopathy remains complex and sometimes overstated. Patients need to approach supplements with caution, prioritizing proven healthcare strategies over unverified claims. Effective diabetes management relies primarily on maintaining stable blood sugar levels, engaging in physical activity, and adhering to prescribed medical treatments. As research continues to evolve, ongoing education remains vital for patients aiming to improve their eye health. Staying updated on scientific findings empowers individuals, allowing them to make informed decisions regarding their health choices. Engaging in regular consultations with eye care professionals can also provide valuable insights into effective preventive care. Furthermore, discussing dietary habits and supplement use in these consultations can help tailor individualized health strategies that suit personal needs. Ultimately, the path to managing diabetic retinopathy involves a multifaceted approach that integrates lifestyle adjustments with medically sound interventions. Therefore, while it is tempting to seek simple solutions through vitamins, it is essential to remain grounded in science. Comprehensive engagement with healthcare resources and continuous self-management remains the best way forward in combating this debilitating ocular complication.
In conclusion, navigating the landscape of vitamins and diabetic retinopathy requires discernment and a balanced perspective. Patients should prioritize evidence-based approaches while remaining open to discussions around nutrition and supplements. This enables a clearer understanding of the roles of vitamins and their limitations in diabetes management. Collaborating with healthcare providers can enhance this journey, ensuring comprehensive eye and diabetes care. Ultimately, the goal remains to reduce the incidence and progression of diabetic retinopathy through diligent management and healthy lifestyle choices. While the quest for quick fixes may persist, focusing on long-term health through informed strategies will be the most effective route for individuals living with diabetes. Therefore, embracing education, adopting healthier habits, and maintaining strong communication with healthcare professionals become vital components of a robust management plan. In doing so, individuals can arm themselves against the impacts of diabetes and retain their vision quality. Consideration of both lifestyle factors and medical interventions should foster a proactive approach to eye health—one that incorporates a collaborative effort among patients, healthcare teams, and ongoing scientific inquiry.
Understanding Diabetic Retinopathy
Diabetic retinopathy is a severe complication often linked to diabetes, which results from prolonged high blood sugar levels that damage the blood vessels in the retina. This condition can lead to vision impairment and, in severe cases, blindness. Individuals with diabetes are strongly advised to undergo regular eye examinations to monitor retinal health, as early detection can significantly improve management outcomes. Signs of diabetic retinopathy may include blurred vision, floating spots, or difficulty seeing colors. As such, treating diabetes effectively is paramount in reducing risks associated with retinopathy. Treatments for diabetic retinopathy can range from laser surgery to injections that inhibit abnormal blood vessel growth. Research continues to explore the relationships between diabetes management, including blood glucose control, and the development of diabetic complications. As lifestyle choices play a direct role in influencing diabetes outcomes, adopting a healthy diet can be fundamental. Ultimately, a holistic approach consisting of lifestyle modification, regular medical care, and education about the disease can support individuals as they navigate the complexities of diabetes and its ocular manifestations.