Managing Blood Pressure Fluctuations During Illness for Diabetics
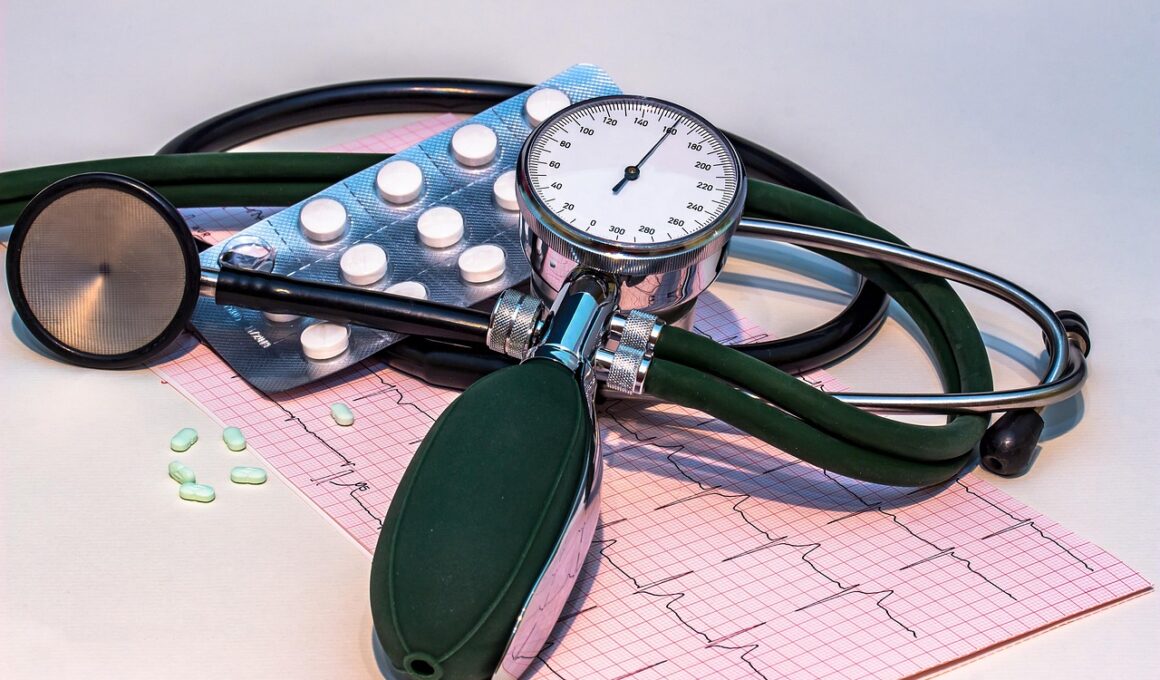
Managing blood pressure fluctuations can be particularly challenging for individuals with diabetes, especially during times of illness. The relationship between diabetes and blood pressure is crucial; diabetics often face a higher risk of hypertension, which can complicate their overall health management. During an illness, factors such as dehydration, stress, and medication side effects can lead to fluctuations in blood pressure. This article aims to guide those with diabetes on effectively maintaining their blood pressure during such challenging times. Knowing how to monitor blood pressure regularly is vital. Patients should keep track of readings during their illness to identify any significant changes. Having a home blood pressure monitor makes it easier to track these readings consistently. If fluctuations are extreme or persistent, consulting a healthcare provider should be a priority. Understanding triggers for blood pressure spikes, like anxiety or infections, can also aid in managing these fluctuations more effectively. Additionally, maintaining a balanced diet and adhering to hydration guidelines during illness can help stabilize blood pressure, ensuring better health outcomes for diabetic patients.
Understanding the Impact of Illness on Blood Pressure
Illness can significantly impact blood pressure levels, and understanding this relationship is essential for diabetics. When suffering from any infection or illness, the body undergoes various physiological changes, which can affect blood pressure. Stress hormones released during illness may contribute to spikes in blood pressure, especially in diabetics. The key is monitoring these changes closely since both high and low blood pressure can pose serious risks. Individuals may experience dizziness or fatigue due to these fluctuations, intensifying health complications. To combat this, diabetics should maintain a well-balanced nutrition plan that supports stable blood pressure. Eating small, more frequent meals might mitigate blood sugar and blood pressure swings. Staying hydrated is equally crucial, as dehydration can lead to lower blood pressure levels. Additionally, managing stress through relaxation techniques or mindfulness can be beneficial. Regular communication with healthcare providers is essential, especially when illness occurs. They can provide tailored advice to manage blood pressure effectively during such periods, ensuring overall better health management through proactive strategies.
Medications play a vital role in managing blood pressure for diabetics, especially during illness. However, some treatments may interfere with blood sugar levels or other medications. It’s essential to consult a doctor regarding any changes in medication. During periods of illness, some may need adjustments to their diabetic regimen to keep blood pressure stable. Monitoring for side effects, such as excessive drowsiness or increased sugar levels, is crucial. Diabetics should keep their healthcare team informed about any medication changes. Maintaining adherence to prescribed treatment plans is necessary for managing blood pressure effectively. Moreover, individuals should document symptoms and medication effects during illness, as this information is invaluable for the doctor. Keeping a clear record can help determine what works best while maintaining blood pressure during sickness. In addition to medications, sometimes combining lifestyle changes can provide enhanced results in managing blood pressure during illnesses. Practicing relaxation techniques such as yoga or deep breathing can help reduce blood pressure levels and promote emotional well-being during stressful times. Encouragement from family and friends can also be vital in motivating adherence to both medication and lifestyle changes.
Diet significantly influences blood pressure fluctuations, particularly for diabetics facing illness. Eating nutrient-dense foods that maintain stable blood sugar levels can positively impact blood pressure management. Including foods high in fiber and low in sodium is often advised. Whole grains, fresh fruits and vegetables, lean proteins, and healthy fats can effectively support blood pressure stabilization. During illness, focus on nutrient-rich soups and broths that are easy to digest may help maintain vital nutrient intake. Hydration should also be prioritized; drinking plenty of water can contribute to better blood pressure control. Minimize caffeine and alcohol consumption, as they can lead to larger swings in blood pressure, especially when the body is already compromised. Portion control is crucial; overly large meals can lead to stress on both the digestive system and overall bodily health, impacting blood pressure. Additionally, meal timing should be adjusted; smaller, frequent meals may be more advantageous during illness. Regularly monitoring blood sugar and blood pressure post-meals helps identify which foods do not work well. This self-awareness can significantly help diabetics maintain overall health during times of illness.
Exercise and Rest Balance
Physical activity often contributes positively to regulating blood pressure, but during illness, this becomes more complex for diabetics. Balancing exercise and rest is essential during this time. While moderate activity, when tolerated, can help stabilize blood pressure, extreme fatigue should be avoided. Gentle exercises like walking or stretching can be beneficial without overexerting the body. However, the focus should primarily be on recuperating energy and slowly regaining strength. Understanding personal limits is vital; if symptoms worsen during activity, taking a break is crucial. Resting adequately contributes to a better recovery and can help normalize blood pressure levels post-illness. Recognizing the signs of dehydration or fatigue plays a pivotal role in determining the appropriate activity level. Furthermore, sleep is equally important; the body requires time to heal and recuperate effectively. Ensuring a comfortable sleep environment can significantly enhance sleep quality. Incorporating good sleep hygiene practices may also support recovery. Balancing activity and rest leads to improved health outcomes, helping manage blood pressure during recovery periods for diabetics encountering illness.
Regular follow-ups with healthcare providers are vital for diabetics managing blood pressure during illnesses. Establishing a line of communication ensures timely medical advice tailored to individual needs. Scheduled check-ups allow for monitoring both blood pressure and diabetes management closely. Patients should feel empowered to discuss their health concerns, enabling healthcare professionals to adjust treatment plans accordingly. These adjustments may include changes in medication, dietary advice, or exercise recommendations based on current health status. Utilizing telehealth options can also facilitate timely consultations without needing to visit the clinic in person. Monitoring both blood sugar and blood pressure at home creates a comprehensive picture of one’s health status. Keeping logs of readings, symptoms, and dietary habits can assist healthcare providers in diagnosing issues swiftly. Enabling individualized care, follow-ups become essential during times of illness, where health management becomes more complicated. Collaboration between patient and provider ensures that both blood sugar and blood pressure levels are optimized, enhancing overall effectiveness in treatment. This proactive approach minimizes risks and ultimately empowers diabetics to take control of their health.
Peer support plays an essential role in maintaining blood pressure stability for diabetics during illness. Engaging with support groups can provide both emotional and practical advice from those with similar experiences. Sharing strategies that worked for others can be comforting and informative. Encouragement from peers can motivate maintaining healthy habits despite challenging circumstances faced during illness. Additionally, utilizing technology such as health apps can connect individuals with support networks and track progress. Social support promotes accountability and encourages adherence to management plans. Diabetics can also find strength in close friends or family who understand their health challenges. Educating loved ones about how to assist during times of illness can prioritize blood pressure management effectively. Involving family in meal preparation or encouraging short walks can enhance collaboration on health goals. Building a robust support system fosters resilience, making it easier to handle the challenges of managing blood pressure during illness. This collective effort equips diabetics with practical tools and emotional support to successfully maintain their health amid fluctuating conditions.
In conclusion, managing blood pressure fluctuations during illness is critical for diabetics. Prioritizing regular monitoring, medication management, dietary considerations, an appropriate exercise-rest balance, routine check-ups, and strong peer support creates a comprehensive strategy. All these elements together facilitate improved health outcomes, minimizing the risks associated with sudden changes in blood pressure. By understanding the specific needs of those with diabetes when ill, individuals can proactively address fluctuations. This holistic approach empowers diabetics to navigate illness more confidently while maintaining their blood pressure within healthy ranges. Ultimately, combining knowledge, proactive strategies, and a solid support system leads to better health management. Taking charge during these vulnerable times demonstrates resilience and determination. To ensure long-term health, continuous learning about diabetes management strategies and incorporating best practices is essential. Regular discussions with healthcare providers aid in making necessary adjustments to treatments and lifestyle changes. Emphasizing self-care and supportive networks reinforces the mindset needed during recovery periods. Empowering oneself with knowledge and actionable strategies ensures that diabetes management remains effective, even during times of illness.