Understanding Blood Sugar Variability
Blood sugar variability is crucial in diabetes management as it influences long-term health outcomes significantly. Diabetes often leads to fluctuating blood glucose levels, affecting both daily life and long-term complications. Oral medications are integral in managing these fluctuations, stabilizing blood sugar levels to prevent the risk of severe hyperglycemia and hypoglycemia. By specifically targeting insulin secretion or glucose absorption, these medications help to minimize variability. For patients, maintaining steady blood glucose levels can enhance quality of life and prevent complications such as neuropathy and retinopathy. It is vital to monitor blood sugar levels regularly and understand their patterns. Medications vary in their action profiles, effectiveness, and potential side effects. Choosing the right oral medication involves considering individual health status, lifestyle, and medication side effects. Increased knowledge about blood sugar variability can empower patients, allowing for more informed discussions with healthcare providers about effective diabetes management strategies. Understanding how oral medications work helps patients to adhere to their treatment plans. Collaboration with healthcare professionals ensures that the risks of variability are managed appropriately.
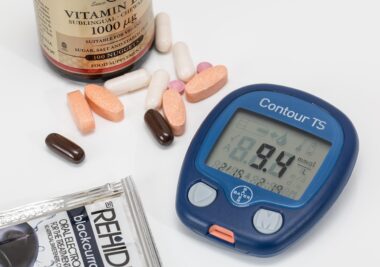
There are various classes of oral diabetes medications available, each with distinctive mechanisms impacting blood sugar levels. Sulfonylureas stimulate the pancreas to release more insulin, effectively lowering blood glucose levels. Some examples are glipizide and glyburide. Biguanides, such as metformin, enhance insulin sensitivity in tissues, which aids in lower blood sugar levels. This is particularly beneficial for overweight patients with insulin resistance. DPP-4 inhibitors work by increasing incretin levels, which promote insulin secretion post-meals and decrease glucagon levels. This class includes sitagliptin and saxagliptin. Another group, SGLT2 inhibitors, reduces glucose reabsorption in the kidneys, leading to increased glucose excretion in urine. Each medication has potential side effects, which is vital to understand for safe management. Additionally, lifestyle changes alongside medication enhance treatment efficacy significantly. Eating a balanced diet, exercising regularly, and monitoring blood sugar levels can further stabilize glucose. Patients should discuss potential side effects with healthcare providers. Achieving optimal blood sugar control is a collaborative effort that not only involves medication but lifestyle management as well. The effectiveness of oral medications is maximized when patients actively participate in their diabetes care plan.
Effects on Glycemic Variability
Glycemic variability can have serious implications for diabetes patients. Studies have shown that increased variability can lead to greater long-term complications such as cardiovascular issues. This knowledge emphasizes the need for medications that not only control blood sugar levels but also minimize fluctuations. Oral diabetes medications can help in achieving this by enhancing overall glycemic control. For example, medications that slow carbohydrate absorption or improve insulin sensitivity may lead to less variability in post-meal blood sugar spikes. It’s important for patients to regularly check their hemoglobin A1c levels, as this measures average blood sugar levels over time, highlighting fluctuations. Medication adherence is also crucial for maintaining stable blood sugar levels. Missing doses can lead to marked fluctuations and complicate overall management. Taking medications as prescribed can support steadiness in glucose levels, benefiting both physical and emotional well-being. Moreover, patients should be aware of factors influencing variability, such as stress, infections, or diet changes. Continuous education about diabetes management and its impacts can lead to more effective self-management and healthier outcomes for individuals living with diabetes.
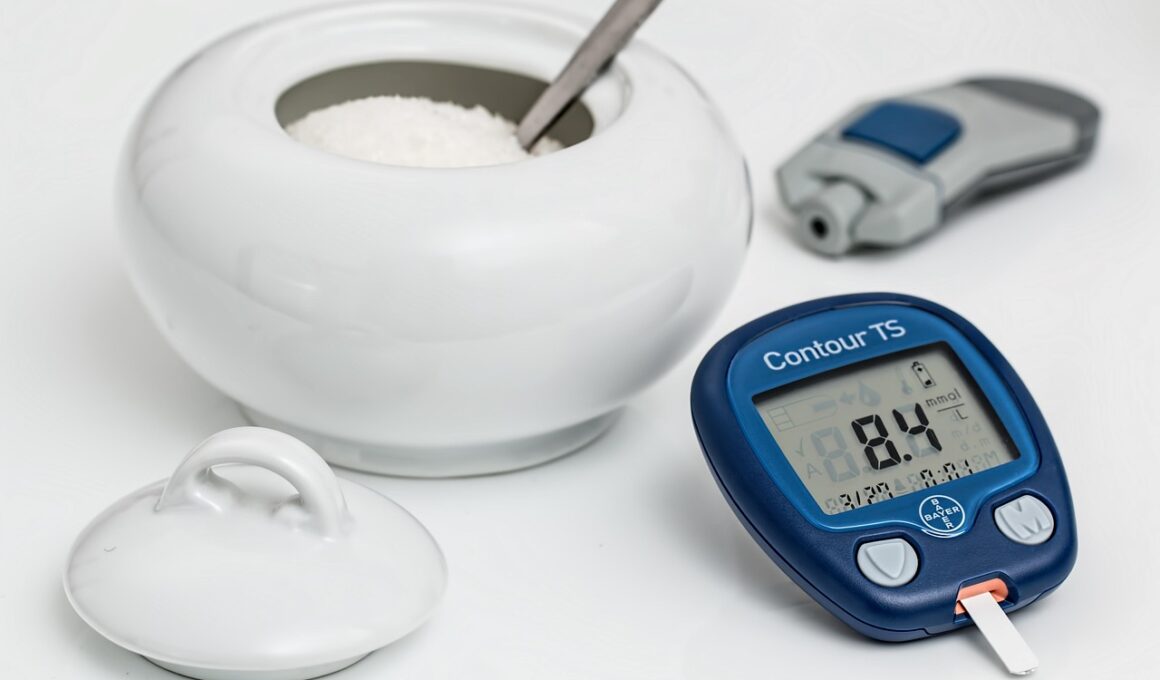
Proper monitoring and assessment of blood sugar levels are essential components of medication effectiveness. Standard blood glucose monitoring methods include home testing via glucose meters and continuous glucose monitoring (CGM) devices. These technologies allow individuals to track their glucose levels throughout the day, providing real-time feedback. By using these tools, patients can understand how different foods or activities affect their blood sugar variability. Furthermore, maintaining a blood glucose diary can help identify patterns that guide medication adjustments and lifestyle changes. Evaluating these patterns can create a comprehensive picture of how medications affect an individual’s glycemic control. Regular consultations with healthcare professionals will ensure medication efficacy is evaluated continuously. They can make necessary adjustments based on monitoring data. Utilizing mobile health applications can facilitate data recording and sharing with healthcare teams, enhancing communication and proactive management. Patients can discuss their logs and insights during appointments, increasing engagement in their treatment plans. Emphasizing the relationship between medication adherence and consistent monitoring leads to better overall diabetes management and reduced risks of complications.
The Role of Diet in Medication Effects
The impact of diet on blood sugar variability cannot be understated, as it plays a crucial role in diabetes management. Oral medications work best when combined with a well-balanced diet tailored to individual needs. Carbohydrate counting and understanding glycemic index can help patients make informed food choices, resulting in more stable blood sugar. Lean proteins, healthy fats, and high-fiber foods should be incorporated to prevent spikes and crashes in glucose levels. Consistency in meal timing also supports medication effectiveness, allowing for predictable blood sugar patterns. Some patients may benefit from the guidance of a registered dietitian to develop a personalized meal plan. This plan can help reinforce the importance of healthy eating alongside medication. Additionally, understanding the interactions between different foods and medications can improve glycemic control further. Dietary education empowers patients to make healthier decisions that complement their medications, enabling them to lead healthier lifestyles. Meal planning, preparation, and mindful eating also contribute to achieving optimal blood glucose levels. The synergy between diet and medication is essential in creating individualized diabetes management strategies that reduce complications.
Considering the psychosocial aspects of diabetes management helps create a holistic treatment approach. Diabetes is not only a physical disease but also affects one’s mental health and social interactions. Patients often experience anxiety or depression related to managing blood sugar levels or fear of complications. These factors can influence medication adherence and overall glycemic control. Therefore, healthcare providers must address these emotional aspects while discussing treatment plans. Support networks, whether through family, friends, or diabetes support groups, can provide encouragement. Mental health professionals can also assist in helping patients cope with the emotional burdens of diabetes management. The relationship between psychological well-being and medical adherence is significant; patients who feel supported tend to be more adherent to their medication regimens. Moreover, understanding the impact of life changes or stressors on blood sugar variability is critical for long-term management. Patients should feel empowered to initiate conversations about their mental health with healthcare teams. Emphasizing the mind-body connection reinforces the importance of approaching diabetes as a multifaceted condition for optimal management.
Future Directions in Diabetes Medication
The future of diabetes management lies in the advancement of oral medications and personalized treatment approaches. Research is continuously evolving, aiming to develop more effective drugs with fewer side effects. The introduction of medications targeting specific pathways involved in glucose metabolism can revolutionize therapeutic options. Beyond medication, technological advancements in monitoring blood sugar levels, such as wearable devices, can provide real-time data. This data will assist healthcare providers in offering personalized recommendations based on individual responses to medications and lifestyle factors. Furthermore, artificial intelligence and machine learning could play roles in predicting blood sugar variability based on historical data. Ultimately, enhancing self-management tools will empower individuals with diabetes to make informed lifestyle choices. This proactive approach emphasizes prevention over reactive management, targeting fluctuations before they escalate. Engaging patients in their care, utilizing technology, and promoting education are crucial steps. Increasing awareness about the importance of managing variability will lead to improved overall health outcomes and quality of life for patients. With ongoing innovation and research, the future of diabetes management is promising and full of potential.
In conclusion, oral diabetes medications have a significant impact on blood sugar variability, influencing overall diabetes management. Achieving stable blood glucose levels is essential for preventing complications and enhancing patients’ quality of life. Understanding the mechanisms of various medications, combining them with lifestyle modifications, and embracing technology for monitoring are essential components of effective diabetes care. Regular consultations with healthcare teams, support networks, and mental health resources contribute to holistic treatment approaches that address both physical and emotional well-being. Research into new medications and personalized care will lead to future advancements in diabetes management. Patients should feel empowered in their journey, actively participating in their care while being educated about their medications. Collaborating with healthcare professionals will ensure a comprehensive and tailored approach that meets individual needs. Ultimately, successful diabetes management hinges on multidisciplinary strategies that incorporate medication, diet, and mental health support. Through continued education and support, individuals with diabetes can achieve optimal health outcomes and a better quality of life.